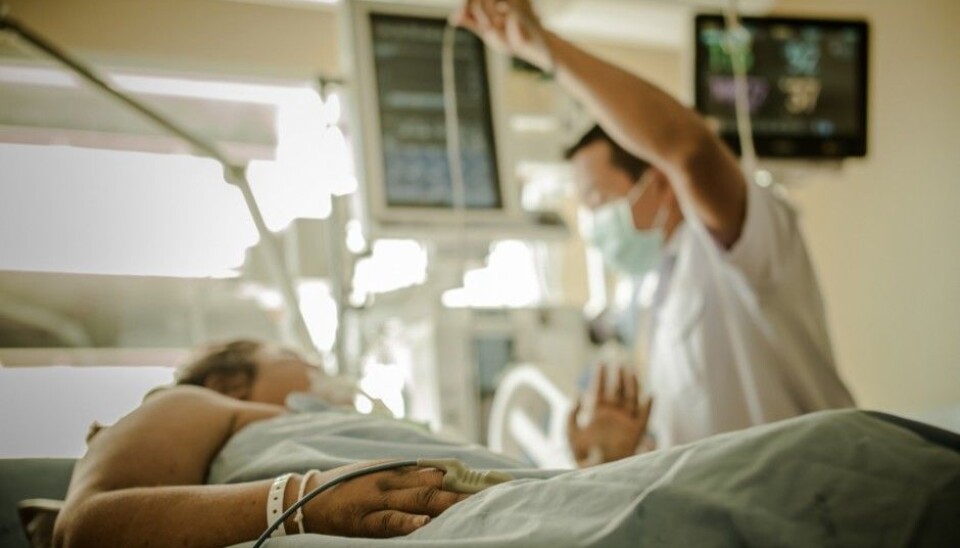
Nurses biased against obese patients
An increasing number of patients entering intensive care units in Norwegian hospitals are obese. Some hospital personnel find it hard to muster the same amount of empathy and provide the same level of care they give to slimmer patients.
“Without a doubt, there are many in the health services who lack understanding that overweightness and obesity are not a moral problem, this is a medical problem.”
So says Mari-Mette Graff at the Norwegian National Association for Obese Persons. She is afraid the consequences can be dire when health personnel point an accusing finger rather than diagnose or give sufficient treatment to sick patients.
Sick people encounter prejudice
Intensive care patients are amongst those in hospitals that are in a sorriest state. They are acutely, critically ill or injured. Many hover between life and death.
Nastasja Robstad has served as an intensive care nurse for many years. She is now working on her doctoral degree about intensive care nurses’ attitudes towards intensive care patients who are obese.
“It is a physical and psychological ordeal to be an intensive care patient. If you also have far too many kilos of fat you can have a greater burden in this situation than a person of normal weight,” she says.
She became interested in the issue because a mounting number of large patients are being admitted to intensive care units. She sees a lack of candour about the attitudes among health sector personnel regarding such patients.
International research has discovered many negative attitudes against fat patients among health personnel. There is also research showing that overweight patients experience being treated differently and that they find encounters with the health services troubling, according to Robstad.
“I was interested in learning what Norwegian intensive care nurses think about overweight patients,” says the researcher from the University of Agder, in South Norway.
Surprised by openness
Robstad’s doctoral dissertation will not be completed until the summer of 2018. But she has published her first article from it. The paper is based on interviews with 13 intensive care nurses from two units at two hospitals.
The nurses are quite ambivalent about obese patients. On the one hand they view them as highly vulnerable persons who need plenty of help. On the other hand they perceive this category of patients as different, difficult and demanding.
“They experienced the admittance of such patients to the unit as something out of the ordinary. The employees use other jargon and express negative attitudes about these patients.”
The nurses find these patients to be physically demanding. They are afraid of injuring themselves when treating them. Such worries can often be manifested as irritation and reluctance regarding the heavy patients.
“Quite a few of the nurses think the obesity is self-imposed. They wonder whether these patients can really expect the same treatment given to other patients. On the other hand, others consider this is a terrible way to think. They feel that all patients have the right to equal treatment, no matter what their weight,” says Robstad.
She was surprised about the candour amongst the nurses she interviewed. Many were glad to have an opportunity to open up with someone about this touchy subject. They wanted to see more light shone on it.
More data needed
Robstad points out that her interviews with 13 persons do not comprise a sufficient basis in data to extrapolate general statements about Norwegian intensive care nurses’ attitudes. She is now continuing her study with some 250 intensive care nurses in 17 intensive care units in Norway.
She is also trying to research both their implicit and explicit attitudes. In other words, she is gauging nurses’ conscious and expressed outlooks and the views they are less aware of.
Unconscious opinions
Researchers know it can be hard to measure people’s real attitudes.
Humans are largely guided by what is socially acceptable to think. So we often answer with what we think is deemed “correct”. This is especially the case with issues that are socially sensitive or touchy. This is why special interpretive tests have been developed that can also catch opinions that are non-verbal. Robstad uses one of these.
Nurses have jobs with stringent ethical guidelines. They know they are supposed to give all patients equal treatment. So Robstad uses a test with a word that appears on a computer screen. Within a milliseconds the person she tests is supposed to put the positive words up on the “thin” and the negative words on the word “fat”.
“The theory is that a person uses shorter time categorising words which one thinks match well than ones which don’t. The quicker the response time to the word “thin”, for instance, the stronger preferences one has for it.”
Robstad also evaluates whether attitudes are having an impact on behaviour. She measures this by presenting terse, common narratives about a patient at an intensive care unit and asks the person being interviewed what he or she would do in the situation.
Irritation over heavy lifts
Although health personnel know of their duty to give everyone the equal treatment, that can require different approaches.
“This is a group of health personnel who work hard and are dedicated. But they are like everyone else. They are influenced by the social norms and attitudes around them, and these are not always so favourable about obese persons,” says Robstad.
“However, this is a very complex issue. Intensive care nurses are afraid of injuring themselves when performing such heavy lifts with these patients. Many get irritated when struggling with heavy bodies. They also often feel they are not getting the help they need from their colleagues.”
Not surprised
Mari-Mette Graff at the Norwegian National Association for Obese Persons is not surprised that research is turning up negative attitudes in the health care system.
The organisation has been notified by patients who have had painful and discriminatory experiences in the primary and secondary public health services.
Graff knows of cases where this could have fatal consequences.
“We have, for example, a woman who rapidly gained a huge amount of weight in the last trimester of her pregnancy. When she visited a doctor she was told she had downed too much marzipan at Christmas. The doctor did not check her blood or urine. It turned out later that she had preeclampsia. This could have had dramatic consequences, a premature birth or even death.”
Fat becomes a filter
Seeking health assistance can be a psychological burden for overweight or obese persons. One example is a woman who visited her gynaecologist. He waited until she had taken off her clothes. Then, and not until then, he said he doubted his examination chair could support her weight.
“Many see only the fat and not the person. The fat becomes a distracting filter,” asserts Graff.
She calls for more awareness in the health sector.
“It is many years since we stopped saying to anorectics that they simply needed to start eating more. But there are still far too many in the public health services who think overweight people can just get hold of themselves and eat less.”
She points out that obesity can hinge upon genes, environment and a lack of knowledge.
“Overeating is now the most widespread eating disorder. I think we also need to talk about this as a class problem. We know that obesity is more common among persons with low incomes and low levels of education. These perspectives are something health personnel lack an understanding of,” asserts Graff.
Health personnel need information
Robstad teaches on this theme to students specialising to become intensive care nurses. She says many are surprised when learning that overweightness and obesity are not just a matter of lacking willpower.
“This is more complicated than a matter of unsubstantial self-control. I think many health personnel need more information about the causes of obesity,” she says.
Robstad hopes her research can help trigger more open discussion about the subject within the health care sector and also remind those who teach health workers to get this across in their lectures.
-------------------------------------
Read the Norwegian version of this article at forskning.no
Translated by: Glenn Ostling
































