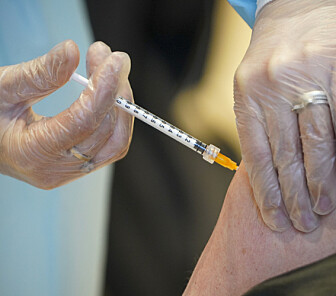
The severely ill elderly should probably not have been given the Covid vaccine first, says vaccine researcher
Not only should we have waited to vaccinate the oldest and sickest, but people in central areas should have been prioritised before the districts, Gunnveig Grødeland believes.
Experts have learned a lot since the coronavirus closed down society and hospitals were filled with patients three years ago, Gunnveig Grødeland believes. She is a vaccine researcher at the University of Oslo and Oslo University Hospital.
The most important lesson, she believes, is that it became clear quite early on that there was a difference in our risk for serious illness and death.
“We should have waited with mass vaccination of all age groups until we had better documentation of the effect,” she says. “The population is not homogeneous. We are many different individuals and groups who have different risks and different benefits from vaccines.”
Grødeland believes we can learn even more from this for next time.
Should have waited with the oldest and sickest
At the beginning of the pandemic, elderly people who were very ill were vaccinated.
“They probably shouldn't have been vaccinated first,” Grødeland says. “We know that vaccines usually have a reduced effect in the elderly, although this vaccine worked better than expected.”
But where to draw the line between when an elderly person benefits from a vaccine and when you might as well not give the shot?
“This is a difficult balancing act,” Grødeland points out.
Could have been more cautious
Geir Bukholm is a professor and assistant director at the Norwegian Institute of Public Health (NIPH).
In an email to sciencenorway.no, he writes that they closely monitored which groups in the population had the greatest risk of serious illness and death. They prioritised these groups first.
The knowledge about this developed throughout the pandemic, and the vaccination strategy was adjusted accordingly along the way, he says.
However, it became clear quite early on that old age was the biggest risk factor.
“Age was the risk factor that alone gave the greatest risk of serious illness and death. But in the very oldest and frailest people, vaccination itself could trigger vaccine reactions that were not appropriate,” Bukholm writes.
At the same time, it is known that the positive, protective effect of the vaccine can be weakened in the elderly with serious illnesses that made them very frail.
“In some contexts, we could probably have been even more cautious about recommending vaccination in this particular group,” he writes.

Believes doctors made good judgments
His impression is that nursing home doctors and other doctors were good at making good assessments.
“A reminder was sent out to nursing home doctors and other doctors to assess the usefulness of vaccinating the very oldest with additional illnesses that made them especially frail,” he says.
Grødeland: Good thing we didn't vaccinate children
In Norway, there was never a recommendation to vaccinate children, even though some groups wanted to vaccinate them as well.
This was correct, as children do not appear to get as sick from the virus as adults, Grødeland argues.
Nor has there ever been a recommendation that people under the age of 45 should receive more than two doses.
And there has never been a recommendation for a fourth dose for those under 65.
“Norway has been rational and has adopted a restrictive approach compared to many other countries. I think this is a great credit to the NIPH,” she says.
“Must dare to prioritise tougher”
Also in the next pandemic, it will take time before a new vaccine is available to everyone. It is important that we learn that we have to use vaccines more strategically in the future than we did this time, Grødeland argues.
“We have to dare to prioritise even tougher in the next pandemic. We should have protected people who live in central areas, Oslo and Bergen first. The risk has been much greater there than out in the rural areas,” she says. “In outer Karasjok in Northern Norway, there is no virus. We knew this from the outset. We should have been tough enough to say so.”
A difficult question
Geir Bukholm at the NIPH believes this is a difficult question.
“The risk of infection was greater in central areas with high population density, while the risk of becoming seriously ill or dying if infected was the same everywhere in the country. This means that vaccinating those with high risk in the central areas first could have had a favourable effect,” he says.
“The next question, however, is: Once you had vaccinated those with the highest risk of severe disease progression in central areas, should you then continue to vaccinate those with medium and low risk in central areas before you started vaccinating high-risk individuals in more peripheral areas?” Bukholm asks. “There is no clear answer to this. Infection-related, vaccine-related, ethical, and political choices are crucial here.”
Was there any point in vaccinating?
Some critical voices still question whether it was unnecessary, or even wrong, to vaccinate the population against Covid-19.
Grødeland points to the clear evidence of the numbers.
“We had weekly reports throughout the pandemic that showed the number of hospital admissions, among vaccinated and unvaccinated individuals. We can see that in the group over 40 years of age, the vaccine had a clear effect on preventing serious illness and death,” she says. “The vaccine was effective. That is absolutely crystal clear.”
When some still are in doubt, Grødeland believes it has to do with the communication of the vaccine’s effectiveness when it was rolled out.
“At that time, there was a good deal of attention on the ability to prevent transmission. But the main task of the vaccine is not to prevent transmission, it is to prevent serious illness. If the authorities had had a clearer focus on this from the start, I think the public would have had a more realistic expectation of the vaccine,” she says.
Was criticised
That the vaccines primarily aimed to reduce the risk of serious illness or death was precisely the NIPH’s message when the vaccines were introduced, according to Bukholm.
“This led to us being criticised for having under-communicated that the vaccines would likely also help prevent transmission,” he writes.
Eventually, data showed that the vaccines actually had a clear inhibitory effect against the first virus variants. This effect became progressively weaker as new virus variants developed.
“If Grødeland believes that the authorities' overall communication in this area fell short, it is of course important to consider this aspect of vaccine communication,” he writes.
Must learn for the next pandemic
It is important to review the experiences from the pandemic and learn from them for the next pandemic, Bukholm believes.
“At the same time, we must expect that the next pandemic will be different from the one we have just gone through,” he writes in his email.
“The infectious agent will probably have other properties and may perhaps affect other groups than SARS-Cov-2 did in the first waves,” he writes. “Therefore, the most important thing must be that we have systematised experiences and lessons before a new pandemic. That way, we are better prepared to make effective assessments that are in line with both the professional and ethical criteria we apply.”
———
Translated by Alette Bjordal Gjellesvik.
Read the Norwegian version of this article on forskning.no