Norway fights back against superbugs
A new national strategy on antimicrobial resistance aims to cut antibiotic use in Norway. But not enough is known about cutting use without compromising treatment, experts say.
Denne artikkelen er over ti år gammel og kan inneholde utdatert informasjon.
Imagine a world where antibiotics don’t work, and a simple infection can kill you. For the 25,000 Europeans projected to die from infections by antibiotic-resistant bacteria this year, that world is here.
“And it will get worse,” says Dag Berild, a senior consultant and infectious disease physician at Oslo University Hospital who has worked on the issue for more than a decade.
A British study from December 2014 puts numbers on Berild’s prediction: by 2050, the report says, more people worldwide will die from infections by drug-resistant superbugs than from cancer.
Berild says the Norwegian government’s new national strategy to address antimicrobial resistance by cutting antibiotic use by 30 percent, adopted earlier this year, has come none too soon. But he warns there is not nearly enough known about how to achieve these goals.
“If we are going to reach the politicians’ goal, it is absolutely critical that we boost research that looks at how we can best cut antibiotic use without compromising treatment,” Berild said.
Much is based on guesswork
Berild says there has been little research funding for this problem, in part because there is little prestige associated with the field. Nor has industry been particularly interested in exploring the problem, he said.
“We currently don’t know the answers to fundamental questions, such as how long a patient should be treated with antibiotics and what doses are best. Today this is based on a lot of guesswork,” says the professor.
One such example is cystitis. This painful bladder infection, for which the standard treatment is a three-day course of antibiotics, drives up antibiotic use among Norwegian women. But must it be treated with antibiotics?
Morten Lindbæk, head of the University of Oslo’s Antibiotic Centre for Primary Care, is involved in a research project to see if cystitis can be treated with painkillers in place of antibiotics, since the infection often gets better on its own. Early results are promising, he said.
Lindbæk believes it’s also important that research on antibiotic use be focused on primary care physicians, who write the prescriptions that account for 85 to 90 per cent of antibiotic use in Norway.
Easier to monitor use
The new Norwegian strategy on antimicrobial resistance will make it easier for the authorities to find out what general practitioners are doing in the doctor’s office.
One of the proposed measures would make it possible to get diagnostic codes for antibiotic prescriptions from the Norwegian Prescription Database. Every time a GP prescribes a drug, the prescription is supposed to include a diagnosis. By being able to see patterns, supervisors can act if a GP seems to be prescribing antibiotics randomly.
Berild says hospitals also need a digital system that can monitor the use of antibiotics by in-house doctors and divisions. A similar system has been used in several Swedish hospitals with success, he said.
Medical tourists and unwanted superbugs
Norway is far better situated than most other countries in Europe in terms of antibiotic resistance, but superbugs are an increasing problem in the country’s hospitals, Berild said.
He thinks the growth in antimicrobial resistance is due both to the over-prescription of antibiotics by Norwegian doctors, and also to the import of resistant bacteria that are inadvertently brought home by Norwegians travelling abroad.
“The further east and south you go in the world, the greater your danger of being infected by resistant bacteria,” he said. “It’s risky to be treated in hospitals in many places in the world, and no one should do so voluntarily.”
He doesn’t think that people should stop travelling, but thinks that medical tourism is risky, whether it is travelling to India for breast implants or to the Baltics for dental work.
Teaching the next generation
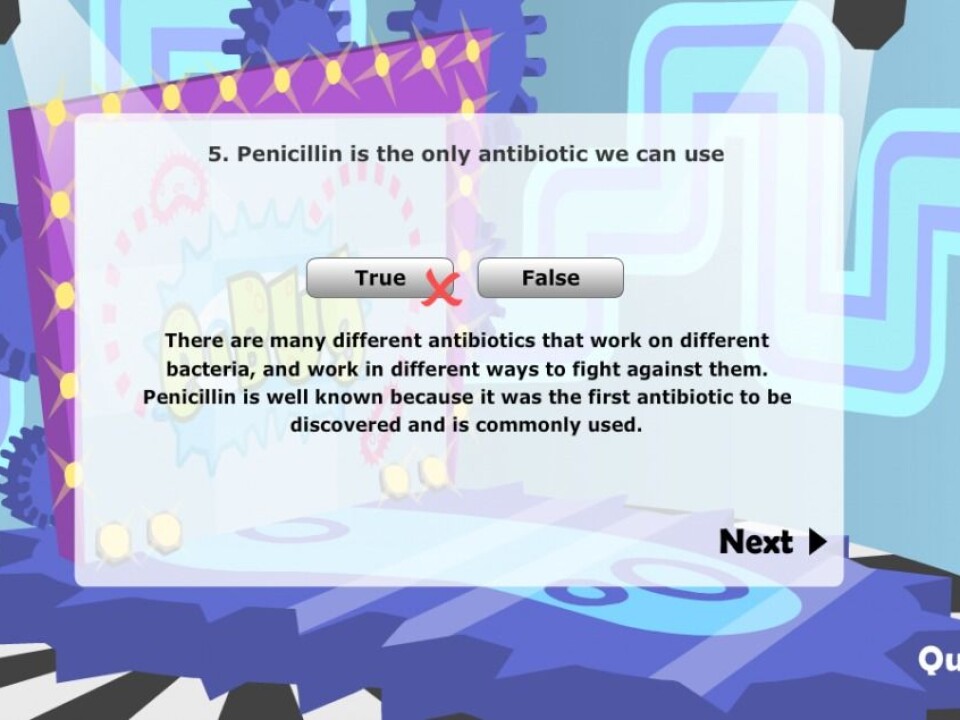
Lindbæk is working with Siri Jensen, a researcher at the University of Oslo’s Department of Family Medicine, on an interactive game about antibiotic resistance called e-Bug.
The program, developed by Public Health England, has been tailored to Norwegian children and will be presented at the Oslo Science Fair during Science Week 2015. It has been used by many European countries that are struggling with antimicrobial resistance problems.
“Our children are the future users of antibiotics. We must teach them from when they are young that antibiotics are a limited resource. When they get an infection, antibiotics should not be the first thing they think of,” says Lindbæk.
-------------------------------------
Read the Norwegian version of this article at forskning.no